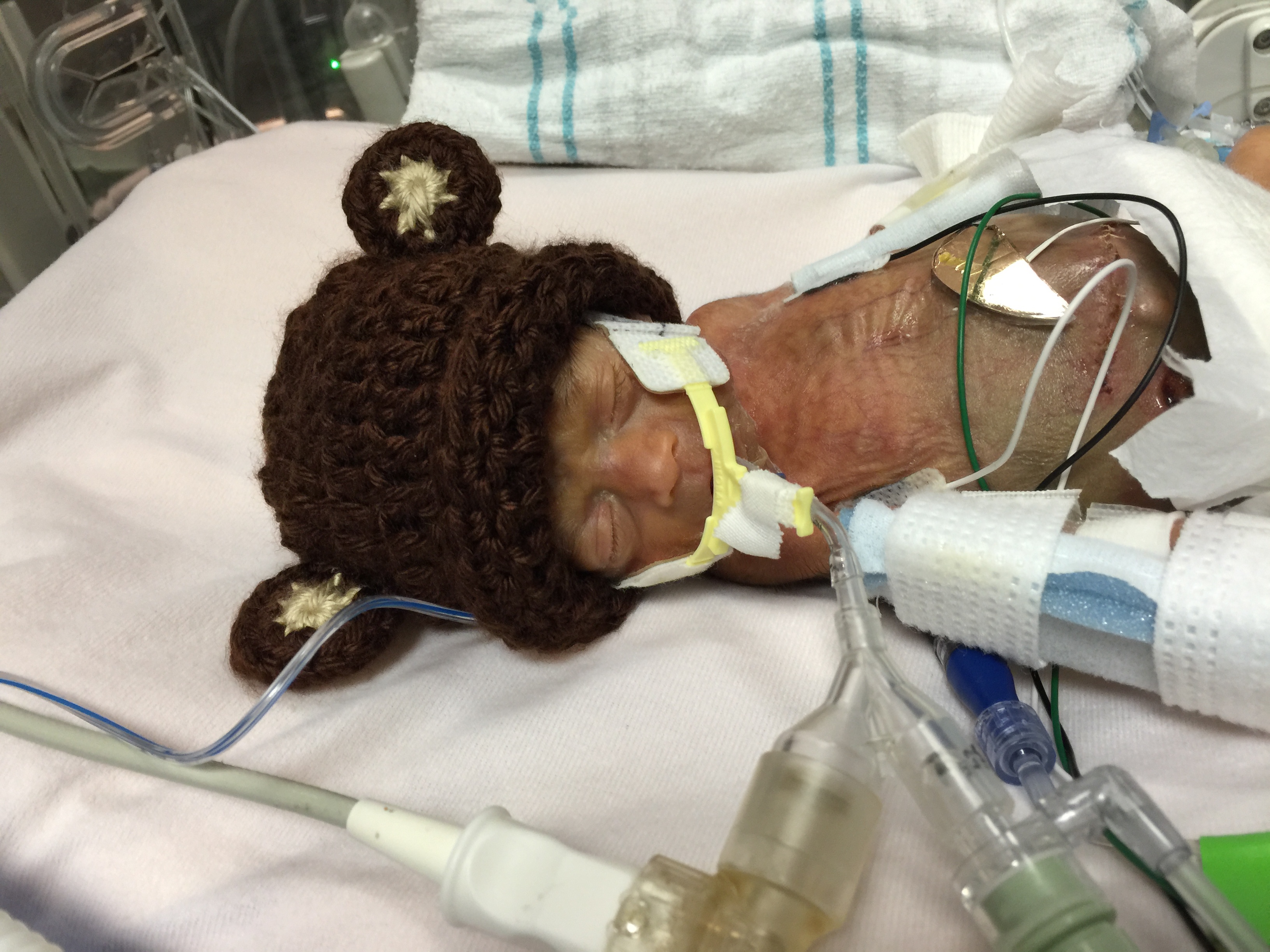
The idea that the NICU experience is a never ending rollercoaster was setting in for us. Never in our lives had we been so exhausted. We were complete zombies and to this day I have no idea how we were able to function during those first several weeks in the NICU. The best example I could compare this feeling to is in movies where a boxer has been beaten down so much, is barely standing and they are about to receive the final blow that will knock them to the ground. We barely came out on the other side of Beckham’s bowel surgery and hearing it was a localized perforation versus NEC was a definite win. This gave us a little boost, as we soaked in the mini victory, but the fight was not over.
Day 11 would bring in a flurry of tests, antibiotics, meds and yet another blood transfusion. Beckham was fortunate enough to be the universal receiver. Now that he was recovering from surgery he would have blood tests daily to check for infection among other things. After all, a bowel perforation was no minor event. Especially one that happened several days prior, blocked itself back up and re-perfed. That meant he had loose stool in his abdomen for several days and put him at extremely high risk for infection. In addition to labs he would need several belly ultrasounds and another brain ultrasound as follow up. His numbers weren’t looking great right off the bat in terms of his blood counts. His H&H specifically, and there was concern of circulation issues in the belly from surgery or a possible intestinal bleed. When his ultrasound of the abdomen came back ok I took it with a grain of salt as the ultrasounds that were taken when he had a perforation never picked it up. Nevertheless Doctors trusted the scans and their thinking went straight to the brain. A brain ultrasound was ordered stat. I didn’t understand it at the time but his physicians where mostly concerned about the amount of stress his body had been through in the days prior. Not just from surgery but specifically the night he almost died and had to be resuscitated several times. This meant he had significant pressure drops and these incidents may have caused a brain bleed. Before the ultrasound the neonatal physician walked us through the grade levels of brain bleeds and what they meant. If there was a bleed then a grade 1-2 was preferable. The lower the number the better and the least likely to have long term damage to the brain. Grade 3-4 were severe and more likely to have long term consequences. These grades could be applied to one side of the brain (Unilateral) or both sides of the brain (bi lateral) so unilateral would also be the better case if a bleed was present. Our immediate question back to the doctors was “well if you do find a bleed then what can be done”? The answer being the last thing any parent wants to hear which is “Nothing”. It has to resolve on it’s own. We would have to watch, wait, and hope for the best, long term, with no real insight into what it could mean for him in the future.
So.. we waited. and waited for results. I was not optimistic. The practical side of me knew there was a reason for the H&H levels to be low, and that it didn’t appear to be surgically related. I tried to shake it off and chalk it up to being irrational or pessimistic but my gut was telling me otherwise. After the wait that felt like an eternity I spotted our NICU doctor with their rolling cart and computer walking over with another physician whom we already knew to be the NICU Neurologist. My heart sunk. All I could do now was to hope for the lowest grade and unilateral results. “Please let this be a ‘nothing’ bleed” I begged internally. The doctor introduced himself and started to make himself comfortable as if he was prepared to stay a while. “This can’t be a good sign” I thought to myself as my mind was running a million miles a minute. I kept thinking “I can handle all the health stuff, but not the brain stuff. Please, I can’t handle a child that will have brain issues.” These words still pain me to type and as I thought them I felt like a terrible human being. The doctor started off by showing us images of Beckhams brain from earlier in the week when he had passed the 7 day brain bleed risk period. This was to give us a visual of what his brain looked like before there was a bleed. He then transitioned over to the imaging from earlier that day whcih showed these enlarged ventricles that seemed to be triple in size. Long black matter amidst the white. That was the bleed. Grade 3. Bilateral… There was some mention of potential pooling of blood in the back of the head as well which didn’t seem significant at the time. The future would prove differently. For now, all we could do was wait. The bleed could take months to resolve, even over a year and would be monitored regularly through ultrasounds. Ultimately we got the answers regarding the blood levels and the reasoning as to why he was needing more transfusions.
The next day hit us like another ton of bricks when Beckham’s blood cultures came back positive for infection. It was expected of course but we always tried to hold onto any ounce of hope which we were beginning to feel like didn’t exist. He was already on 2 antibiotics and a third would now be added. The doctors were debating doing a spinal tap to ensure the infection wasn’t headed for the brain but a spinal tap with a brain bleed was quite risky. They opted against it. The blood cultures showed the infection was Enterocaucus and he would now require cultures to be taken every day. This was no small feat for a now 1lb 9 oz. micro preemie. He needed to hold onto every drop of blood in his body. With so much going on he would require frequent transfusions of both blood and platelets. A new team, known as the infectious disease team, would be on his case and making rounds every day in addition to the surgical, GI, Pulmonary, neurology, and neonatal teams that were already on rounds for him. These were just the core physician teams. At this point it seemed like Beckham didn’t have anymore space on his body for all the lines running to and from him. He was completely surrounded with oxygen, feeding tube, med line, transfusion lines, heart monitor, pulsox and soon would have an ostomy bag added to the site of the resected bowel now protruding from his stomach. All of this on a baby that weighed as much as an apple, inside a heated incubator as at this gestation his body was unable to regulate it’s own temperature. We waited anxiously every minute for new results. For something to come back negative, for that ounce of hope we kept believing would be there for us. Anything would be a victory at this point whether it was weight gained or oxygen sustained. There had to be a light at the end of this never ending tunnel of hell. A few days later that light we had been waiting for would finally be given to us.