In the NICU there is no future, there is only present. It’s important for parents to adjust to this mindset of not being able to plan for their baby’s milestones or going home date because it will only lead to more and more disappointment. Easier said than done. As a project manager this was one of the toughest adjustments for me being in the NICU. I am a person that likes complete organization, to have things planned out and if anything changes all hell breaks loose. How can I not think about my baby’s future? Honestly, a tough adjustment mentally but emotionally it was easy. If I began to think about what the future held for my baby I would just start crying, so essentially it required me to create a mental block and focus on the now.
When walking into the Texas Childrens NICU level 4 we had no idea what to expect. I just assumed there would be tiny babies everywhere. Our eyes were opened to a whole new world of medicine, technology, tragedy, success stories and more. When we walked in, two sinks were to our right and cubbies to our left. Every day going forward we would have to stop, wash and sanitize. We were then taken through a dark noisy space full of pods labelled by letters and bed spaces with numbers. I couldn’t see anything else as we walked in and were directed to D69. As we approached to see him lying in a glass incapsulated incubator I noticed I could see more wires and stickers and tags than I could see baby. His incubator was surrounded by monitors and screens. Everything made it’s own alarm noise or pumping noise. The NICU was a surprisingly noisy place. I looked around, to see there were no rooms, no doors, only an open room with the bed spaces of babies around us just feet away. Tears filled my eyes. I stared at my baby boy and placed my hand on the warm glass. His incubator was not only temperature controlled but also humidity controlled as their skin is extremely fragile. Something as small as a pulsox band placed onto his foot would pull his skin off when removed. The heat was needed to maintain the baby’s temperature as a 24 weekers body is not capable of doing so. The day quickly became a whirlwind of information as we met our nurse, our respiratory therapist and our doctor who stayed with us by the bedside with her mobile computer unit. I was told to get a notebook to track Beckhams stats day to day and it would help me to follow and better understand everything that could happen. The first week is sort of a honeymoon phase. Things can go really well up until they don’t. Essentially waiting for the shoe to drop. The first week is brain bleed watch. Once Beckham could reach 7 days with no brain bleed he would be essentially in the clear. Brain bleeds are grade 1-4 with 4 being the worst. They can occur on one or both sides of the brain and the severity also can indicate the range of complications short and long term. They would schedule his first brain ultrasound. His lungs would also be a big priority as they were extremely underdeveloped and when babies come out this early oxygen exposure for premature lungs could and most likely would cause some damage and he would most likely develop BPD or chronic lung disease. He had already had one chest X-ray and would have another. Over and over again we heard the words roller coaster. Everyone referred to this experience in the NICU as a roller coaster. Already we had stepped onto the scariest roller coaster of our lives and this day felt like the worst part of it.
We were walked through what Beckhams schedule would be, all of his risks, and lots of terminology. Micro preemie is what they called him. Micro preemies are the tiniest of the preemies and the most at risk. They typically range from 23-26weeks in gestation and under 2 pounds in weight. Beckham was at the smallest end of the spectrum of being a survivable baby. 24 weeks. 24 weeks is typically considered survivable and while babies can survive at 23 weeks it’s less likely. He was initially weighed at birth at 680 grams translated to pounds as 1 pounds 8 ounces. The doctor explained that, as most babies do, he would lose weight and the goal would be to minimize any weight loss. I couldn’t imagine him losing weight or being any smaller than he was already. Not only was he tiny but he was not the chubby, rosy cheeked baby that moms deliver close to their due date. He was skin and bone. There was no fat to be seen, to the point that we could see every rib in his rib cage. He was tiny and sickly looking. His face resembling that of someone who had lost weight too quickly, skin slinking down his face. It wasn’t until then that I realized I had not seen his eyes. The nurse informed me that many babies at this gestation still have eyelids that are sealed shut. We could expect him to open them within the week. The more I stared the more I realized all of the things he still had yet to develop. Little things like hair on his body, nails on his fingers and toes, his ears were tiny but not completely finished forming, not to mention all of the things inside that would not have been finished developing. His eyes, certain organs such as lungs and the liver would need to be checked and monitored. So many things to consider, so much information about the human body and its function as it develops that we had to absorb and comprehend. One day at a time, we were told, we will take things one day at a time.
As we started to communicate what was going on and the situation with close family and friends it was difficult to express our joy of our sons birth. His life hanging on by a thread, we were not capable of feeling the excitement of having a son, in fear that if we embraced this happiness and love for him that we would soon enough lose him and the attachment we would develop could rip our hearts out. As much as I would like to say we stayed by his side every minute of that first day, it wouldn’t be honest. We needed to step out, take a break, breathe, and eat. Our parents would show up and provide comfort and food, forcing us to eat as we really could not stomach much. I made phone calls to few and with every call I would cry more and more. Everything else went to voicemail. I couldn’t think of speaking anymore. To this day I still have every voicemail saved on my phone from that day, including the one from our surrogate. I can’t let them go.
The NICU staff escorted us to the Ronald McDonald House, thankfully located on the same floor as the NICU. I had never realized they had locations within hospitals. We were welcomed warmly and ask to fill out paper work. We would automatically get a room the first night as a new patient and from then on rooms were given on a patient severity basis. The tour was short as we entered a small community living space. To the right were some computers and printers which I didn’t know at the time how often I would be using for the mounds of paperwork for insurance and medicaid etc. we would deal with. To the left the kitchen, where occasionally meals were provided and where we could store our own personal food items. There was also a community laundry facility with 1 washer and 1 dryer and supplies were provided. The volunteer unlocked the door as we entered a hallway that resembled every aspect of a hotel. The rooms were all exactly the same. Each room had a queen sized bed, a bathroom and a desk. Soaps and shampoos piled in a small basket came in all different shapes and sizes as people donate their unused hotel bottles. We would need to pick up our room key by 9 PM and check out by 11 AM. We would also be able to reserve space during the day for 1 hour for naps or showers. When we would enter the room we would need to make our own bed and towels were provided for the shower. On the desk there would be a blue garbage bag and before we checked out we would need to unmake the bed and place all linens and towels in the bag outside of the room door and then return the key. It felt like being at a camp, especially the blue plastic water resistant mattress’. The last portion of the tour we were taken up a few steps to an outdoor garden. It was a small space with tables, chairs and benches, colorfully decorated bird houses and tiles and fake flowers all done by children who had or were currently occupying the hospital.
As we made our way back to Beckham’s bedside I felt relieved to see nothing had changed. Every moment we stepped away I was anxious. The first rule of thumb in the NICU stressed to us by the doctors and nurses was to not look at the monitors. Knowing this we never took our eyes off of them. His oxygen levels, heart rate and blood pressure were all on one monitor while his respiratory rate and various other breathing levels were on the other. Above the incubator was also a temperature and humidity level monitor which would sound an alarm if he was too warm or too cool. We didn’t yet understand the respiratory details so we watched his HR, BP, and O2 non stop. His blood pressure was an average between the two numbers. His average needed to remain at or above his gestation, therefore 24+. He ranged anywhere from 22-25. If he dipped he would be given meds such as caffein, and dopamine. He was also receiving TPN, multiple antibiotics and surfactant which was a lung stimulant. We learned that day that Beckham would be at more risk with his lungs because our surrogate was not given steroids before he came out and these would have greatly benefitted him. There just wasn’t enough time, he came out too quickly…
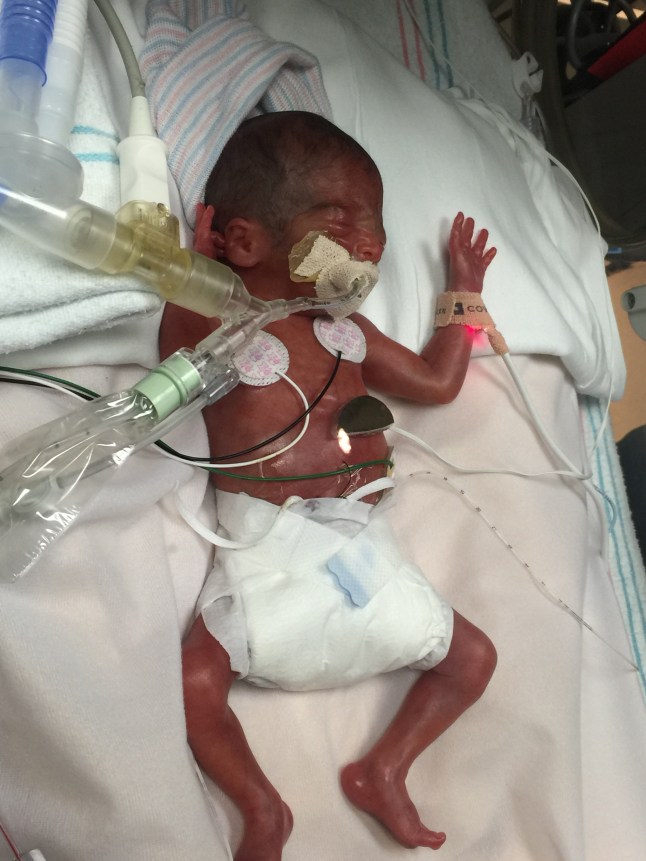
As we neared the early evening and were mentally, emotionally and physically drained, our nurse asked us if we would like to change his diaper. I immediately got up and said “absolutely!”. Anything to have physical contact with him and positive moment for the parents. Josh said he would watch, he was still too scared to touch this incredibly fragile being. It wasn’t easy. To maneuver him so delicately and change a diaper the size of a credit card was scary. The diaper was double the size that he needed but it was the smallest they had. I couldn’t lift his legs too high as it could cause a brain bleed, and touch had to be extremely delicate with his skin so it did not tear. Additionally the change needed to be done quickly so that we didn’t let out too much heat and humidity and light. Unless he needed something to be done, going forward, he was to be treated as if he were still in the womb. A cover would remain over the incubator, noise levels needed to be as non existent as possible and touch times would only occur for the quick check ups every 3 hours. More information to absorb. Luckily we had nurses to remind us of these things several times knowing it was day 0 for all of us. That night even though we had a room, I never left his bedside. I couldn’t bear the thought of not being by his side if something happened. As the night team arrived and we had eaten and I was on the verge of passing out when the new nurse told me “you know, your son is the smallest baby in this entire hospital right now”. He would continue to be the smallest baby in the entire hospital for months to come.
#TEAMBECKHAM



of course you watched the monitors. I imagine that shock carried you through quite a lot of the initial days. Rather glad for the routine you had at the Ronald McDonald House rooms. A bit of semi-normal physical work, the bed changing etc, is a good way to help anchor the mind.
LikeLiked by 1 person